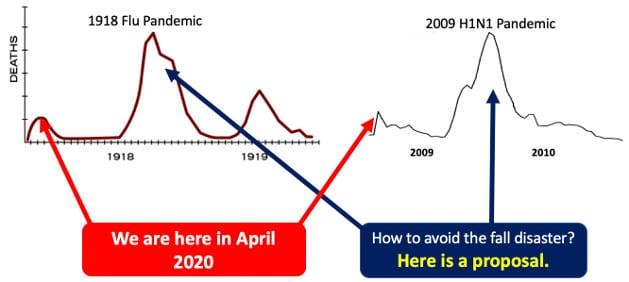
Proposal on how to avoid fall resurgence of the COVID-19 health crisis. Chart courtesy of Dr. Cliff Han
By DR. CLIFF HAN
Los Alamos
With all the talk of flattening the coronavirus pandemic curve of infections, we can also ask the question another way: When should we raise the curve?
This accompanying chart is one we’re all used to by now: showing the number of newly infected people during the course of a pandemic. The CDC is currently trying to flatten the curve with preventive measures so that the pandemic will not overwhelm the healthcare system. But, if the priority is saving lives, then actually raising the curve at the right time should be the strategy; that is, allowing the number of infections to climb. The right time is from late spring to the end of summer when higher temperatures will make the pandemic mild with fewer fatalities.
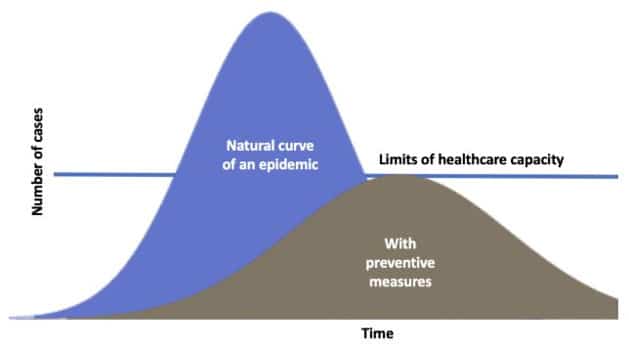 Chart showing the number of newly infected people during the course of a pandemic. Courtesy/Dr. Cliff Han
Chart showing the number of newly infected people during the course of a pandemic. Courtesy/Dr. Cliff Han
Temperature plays a key role. When I was growing up in China, we lived in a house with no heat. Both of my grandparents had severe chronic bronchitis for all of their lives, especially in winter. The condition was so critical that it eventually contributed to their deaths. My mom also suffered from chronic bronchitis up until she was 50. When we moved into a house in the city with heat, her infection went away. Her recovery seemed like a miracle, but it was merely the result of staying warm in the winter.
That’s because the optimal growth temperature for probiotics (good bacteria) is between 85 degrees and 98 degrees Fahrenheit, and our average body temperature is at the top end of that range. Though they are generally beneficial, too many probiotics may reduce our immune defense. While we’re warm, our body fights viral infections well. But when we get cold, our probiotics and immune system are imbalanced and don’t work as well. Viruses like the common cold, flu, and very likely coronavirus have a better chance to take root, multiply and cause trouble.
A similar pattern can be seen with the 1918 Spanish Flu. It had three waves, with the second and third being much more lethal. At the start of March 1918, a troop of soldiers became infected. As they deployed in Europe, they spread the virus through the cold spring. But, by the time it reached Spain in May, the warmer temperatures strengthened people’s probiotics and immune systems. Patients could clear the virus more efficiently, and there were fewer deaths. The mortality rate became so low that people thought the pandemic was over. That belief changed with the seasons. The second wave hit the colder, northern populations, and a medical system already strained by World War I was overwhelmed with thousands of severely sick patients.
Does COVID-19 behave the same as the common cold and flu, and will it become mild in the summer? Very likely.
Recently, New Zealand, following Australia, announced a one-month lockdown. I was curious and checked their numbers. I found 200 cases and 0 deaths in New Zealand and 2,364 cases and eight deaths in Australia March 23. The death rate in the two countries is below 0.4 percent, which is half to one-twentieth of the scale in other countries. Australia and New Zealand are at the end of their summer. The pandemic in that region is a lot milder than it is in Europe, China, and the U.S.
Of course, New Zealand and Australia have their unique situations. Australia has been testing robustly. It may have the highest per capita testing rate in the world. Let’s consider other warm regions much more significant than those two countries and also consider Europe, where it is cold. Europe has a population of 741 million and 575,108 cases of COVID-19, with a fatality rate of 7.4 percent April 2.
South America has a total of 422 million people and 21,378 infected cases, with a fatality rate of 3.2 percent. Africa, with a population of more than 1.2 billion, has only 7,237 cases, with a death rate of 4.2 percent. Pandemic in these two continents started later than in Europe, and are showing a slower progression and lower death rate. Other factors may cause part of the difference. However, both South America and Africa have had warmer weather since the beginning of this pandemic than Europe.
Finally, let’s compare COVID-19 in South Korea and Singapore. Both countries have many things in common. They got their first cases before the closure of Wuhan. They have been using rigorous and practical approaches to control the epidemic, resulting in a similar total number of cases relevant to their populations. The significant difference is that South Korea, where it has been colder, has a death rate almost three times higher than Singapore, 1.7 percent compared to 0.5 percent.
We may conclude after these comparisons that COVID-19 behaves similarly to the common cold and flu and becomes mild in warm seasons and regions. What should we do if the climate can change the course of the pandemic so dramatically? One possible strategy is called “herd immunity.” This is when a population has enough people who have natural immunities to the virus that if an infected person is introduced, the disease won’t spread very far. The “herd” is immune. While now is not the right time to try this approach in the Northern Hemisphere (in fact, the United Kingdom considered and then abandoned the idea) because so many countries and regions are still experiencing cold weather, the timing is coming with the warm spring.
Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, said on April 5 that the coronavirus is unlikely to be completely eradicated from the planet this year, and it may come back next flu season. I would say there will very likely be a visible circulation even in the summer before a significant portion of the population has immunity. We should not wait for another disaster to happen in the coming fall. We can manipulate this summer’s mild pandemic to our benefit.
Trying to avoid repeating the 1918 flu disaster by flattening the curve is the right move for most countries in the Northern Hemisphere for now. But, that needs to change as the months pass. We should increase flattening measures in the fall and winter to save our hospitals from being overrun. Still, we should be relaxing those measures in the spring and summer to generate that needed herd immunity when our airway defense is more robust and to let the vast majority of people get back to work and live relatively healthy lives.
Two facts support this proposal. First, as long as the temperature remains warm, the pandemic will stay gentle. Second, a human-made vaccine is at least 12 months away, but COVID-19 waits for no cure. It will continue to spread over those months. Keeping the entire planet’s population locked up for a year will be devastating for jobs, food supplies, and infrastructure — not to mention everyone’s mental and emotional well-being.
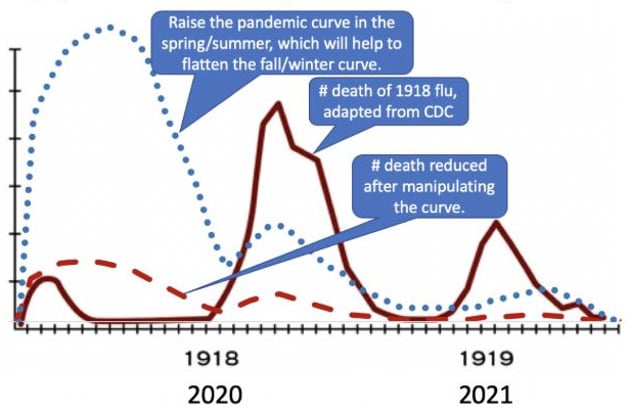
Raise the curve from mid-late spring to late summer when the death rate is low, so that more people become immunized. Then the curve will be flattened in the fall-winter automatically when the death rate is likely to be higher. This approach will have a much smaller impact on normal life and the economy than other alternatives. Courtesy/Dr. Cliff Han
How many lives will this approach save? At this early stage, such numbers are impossible to state for sure, but I estimate it would save between 50 percent and 90 percent of the lives now being lost, based upon current data.
How can you help save these lives?
- Share this proposal with your family and friends through your social media.
- Write a letter to your congressman, senator, and encourage them to examine this proposal.
- Send the blog to your local newspaper.
- Recommend to your local health official and discuss it with them.
COVID-19 will most likely continue to spread until the majority of the population is immunized, naturally, or through vaccination. Raising the curve with a much smaller loss of life may be the only option. Also, we may finish the pandemic by the end of this summer if we speed the epidemic enough and produce sufficient herd immunity against the virus.
Editor’s note: Dr. Cliff Han is a former medical doctor who has been a biologist for 28 years and was a team leader at the Los Alamos National Laboratory. The author of more than 300 research papers, he is the inventor of AllerPops prebiotic lollipops, formulated to provide long-lasting relief to allergies by introducing “good” bacteria to the immune system.

